Feeling lightheaded off and on throughout the day
A 64-year-old female presents to the emergency department (ED) with “feeling lightheaded off and on throughout the day.” She describes herself as a healthy woman with an active lifestyle. When she got out of bed this morning, she noticed that she was dizzy, but it was gone by the time she was dressed. Throughout the day she has been having periods of dizziness that last from several seconds to several minutes. This culminated in a syncopal episode while preparing to leave work. An ambulance was called and she was brought to the ED.
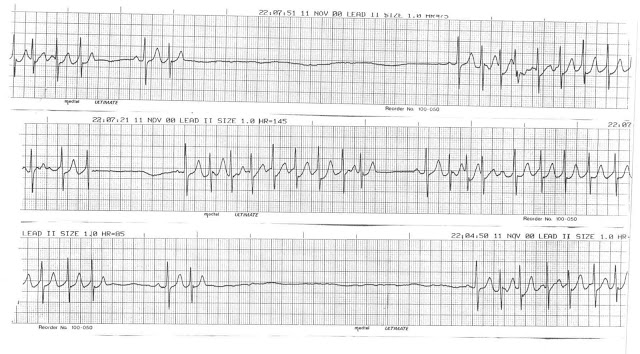
Exam: Healthy, well-nourished 64-year-old female. Her skin is warm, dry. Lungs: Clear Pulse: strong but irregular R: 22 with an oxygen saturation of 96% on room air. Her only past medical history is high cholesterol for which she takes Lipitor 10mg q day. She also takes ASA 81 mg q day prophylaxis. Abdomen is negative. The patient is placed in a room and on the cardiac monitor. Her rhythm strip is as follows:
This ECG represents tachy brady syndrome (AKA sick sinus syndrome). This occurs when there is sinus node dysfunction that inhibits the node’s ability to maintain a steady heart rate. The result is alternating tachycardia and bradycardia. The symptoms of this condition are caused by the sudden changes in heart rate and can include dizziness, syncope, palpitations, diaphoresis and chest pain. This patient needs to have a number of diagnostic tests before a treatment regime can be determined. Laboratory studies looking specifically for electrolyte imbalances, echocardiogram to evaluate heart size and function and either stress testing or cardiac catheterization to determine the presence of underlying coronary disease. If any of these are positive, the underlying issue is treated and the arrhythmia should terminate. If diagnostic testing fails to find a cause or the correction of underlying issues does not terminate the arrhythmia, then the placement of a pacemaker must be considered.
Written by Judith Haluka on Oct 15, 2017
Last reviewed and updated by Caitlin Goodwin on Oct 15, 2017